Celiac and type 1 diabetes
Disclaimer:
Please note that no content on this blog should ever be used as a substitute for direct medical advice from your doctor or a qualified clinician.
What is Celiac disease?
Celiac is an autoimmune disease where the small intestine is affected by gluten intake and the body is unable to absorb a protein called 'gluten' which is found in wheat, rye and barley. When a person with celiac consumes gluten, the body attacks the lining of the small intestines thus making the process of digestion difficult. In the long run, undiagnosed and untreated celiac can permanently damage the small intestine and prevent nutrients from being absorbed.

It derives its name from the Greek word “koiliakos” after the Greek word “koelia” (abdomen). An ancient Greek physician, Aretaeus of Cappadocia while giving it this name said, “If the stomach be irretentive of the food and if it passes through undigested and crude, and nothing ascends into the body, we call such persons coeliacs”.
Untreated celiac may lead to :
- Osteoporosis
- Anaemia
- Infertility
- Organ disorders
- Delayed puberty
- Stunted growth
- Inability to gain weight
- Weak tooth enamel
- Seizures
- Depression
Celiac affects about 1% of the world’s population, however the prevalence of this autoimmune disease amongst type 1 diabetics is very high.
Almost 6 % of T1s also have celiac.
When I met my endocrinologist for the first time, the first thing I got tested for was celiac.
Causes of Celiac Disease
There aren’t exact known causes of celiac. Most researchers believe multiple factors are responsible, like genes, environment, and the foods you eat. You need some or even all these factors to be present to develop celiac disease.
Celiac is autoimmune, however research has suggested that people with a first-degree relative with celiac (parent, child, sibling) have a 1 in 10 risk of developing celiac.
Symptoms
Celiac can be difficult to diagnose because it affects people differently. There are more than 200 known celiac disease symptoms which may occur in the digestive system or other parts of the body. The common symptoms of celiac are:
- Gas
- Abdominal pain
- Diarrhoea
- Constipation
- Cramps
- Nausea
- Indigestion
- Foul smelling stools
- Bloating
- Memory problems
- Hair loss
- Anxiety
- Low blood sugar
Besides these, few people also develop Dermatitis herpetiformis, a severe skin rash associated with celiac.
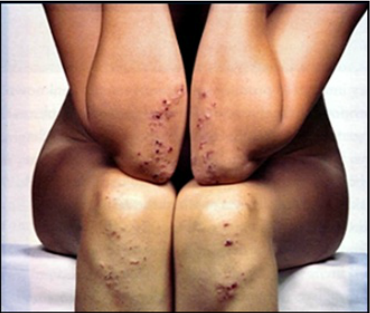
Mostly the diagnosis of celiac is done in childhood however few people are asymptomatic and are diagnosed as adults. Another interesting fact is that mostly people are diagnosed with T1 first and celiac later, which is why we are recommended to get screened for celiac every year after diagnosis. Read our checklist for routine tests here.
However this isn't a set in stone rule. Kashni, is a 13 year old girl who was diagnosed with T1D 2 years ago. In my conversation with her lovely family, I learned that she had celiac way before she was diagnosed with T1D and had been displaying symptoms of celiac since childhood. Due to lack of awareness, she went undiagnosed until her T1D diagnosis. Today she manages her T1D and celiac very well with changes in her diet.
Diagnosing celiac
To diagnose celiac, a simple blood test can help. This test checks the levels of antibodies in a person’s body. A person living with celiac will have higher number of antibodies.
The diagnostic test for celiac is called IgA Anti TTG test.
For this test to be accurate, the person being tested needs to be on a gluten diet.
As per the Celiac Disease Foundation, the following people should get tested for celiac disease:
- Children older than 3 and adults experiencing symptoms of celiac disease.
- First-degree relatives of people with celiac disease – parents, siblings and children have a 1 in 10 risk compared to 1 in 100 in the general population.
- Any individual with an associated autoimmune disorder or other condition, especially type 1 diabetes, thyroid, autoimmune liver disease, Down syndrome, Turner syndrome, Williams syndrome, and selective immunoglobulin A (IgA) deficiency.
In case you experience any symptoms, please connect with your healthcare provider for the requisite steps.
Treatment
The only known treatment for managing celiac is going on a gluten free diet for life.
Celiac and T1 - double edged sword
Diagnosis for celiac is relatively more difficult than T1D, particularly for T1s, since the symptoms of both these diseases overlap, a lot of people go undiagnosed for celiac.
Since T1s are at a greater risk of developing celiac, it's important to get screened.
Gluten free foods and BG impact
Once diagnosed, and after starting a gluten free diet, the intestines start the healing process, however it's slow. T1s have reported more stable blood sugars after being put on gluten free diets because gluten prevents the absorption of carbohydrates in the intestines, which often causes unexplained blood sugar highs and lows.
One of the major parameters of managing T1d successfully is carb counting. High carb foods and high GI foods are best avoided to manage diabetes well. To manage celiac well, a person needs to be on a gluten free diet for life. This may lead to contradictory dietary requirements for a person. For e.g.: the alternative for gluten could be corn, which is a high GI food and hence not suitable for type 1 diabetics as it could lead to a sharp rise in BG levels. Finding food options that work well for both the diseases can be difficult.
Dealing with this dilemma can be made easy by eating a low carb diet.
A low carb diet means there would be no wheat, rye or barley intake. Depending upon your food choices of being a vegetarian or non-vegetarian, you can research and find food items that are low carb and gluten free.
In my interaction with Kashni's mother she told me that Kashni mostly eats besan and avoids eating refined flour. She eats fruits too. Her family buys gluten free flour from a store called 'Goodness Store' in Gurgaon. It would be great to find a local store around your area that can make gluten free flour for you.
Eating out with T1 and celiac
As type 1 diabetics, when we learn the ways of self-management, we teach ourselves the art of eating out. I personally love eating wheat-based pastas and pizzas to avoid eating foods made with refined flour. However, that’s a disaster waiting to happen for a person with celiac. It’s very important to talk at the restaurant well in advance to avoid any adverse reactions. Gluten can also be transferred from containers in which food is cooked thus causing an allergic reaction.
Reading labels of packaged foods is an important aspect that we are taught as diabetics, similarly it's very important that people living with celiac also learn to do it. Please keep in mind the following points for reading gluten free labels:
1. Consider naturally gluten free foods
Naturally gluten-free foods (like bottled water, carrots, unflavoured rice) may or may not necessarily be labelled gluten-free. This does not mean that these products contain gluten or have come in contact with gluten.
2. Connect with the manufacturer
In case you are unsure of the ingredients, please get in touch with the manufacturer to find out.
3. Read ingredient lists carefully
Look for wheat, rye, barley, and their derivatives, like (barley) malt. Understand which products are at a highest risk for cross-contact with gluten.
Challenges
Besides the above, complete removal of gluten-containing grains is challenging. Hidden sources of gluten may be found in the ingredients of many processed foods in the form of additives, stabilizers, thickeners, flavorings, extracts, emulsifiers, hydrolyzed textured vegetable proteins and certain ground spices. Even if you are cooking at home, besides having a separate set of utensils for cooking, an in-depth study of all ingredients being used in cooking would really benefit.
Another challenge, particularly for type 1 diabetics is that we carb count and take insulin doses accordingly. It's very important that dietary requirements are met with what we eat. We must consider our protein and dietary fiber intake. This poses a challenge because many processed gluten-free foods are high in carbohydrates but low in protein and fiber.
Tips to remember
- Work closely with with a knowledgeable and credentialed dietitian (registered dietitian and/or certified diabetes educator).
- Many gluten-free flour substitutes are much higher in carbohydrate content than their gluten-containing counterparts. Gluten-free products tend to be highly refined and contain added sugars or starches. Being T1s, carb intake needs to be monitored properly and hence insulin doses need to be altered to make sure that both conditions are managed properly.
- Some gluten-free alternatives are made with very low-carbohydrate substitutes, and thus standard carbohydrate counts are not appropriate.
- Always keep gluten-free food /snacks with you for managing blood glucose for emergency situations where gluten-free foods may not be easily available.
Busting celiac myths
Just like we did for type 1 diabetes, lets bust some celiac myths for you :
Myth 1: A person with celiac disease can tolerate a small amount of dietary gluten once in a while.
No, this isn't true. While a person with celiac can tolerate a small amount of gluten, it is still damaging the intestines and might not be good in the long run.

Myth 2: Celiac disease can be outgrown.
Just like T1, celiac is life-long.
Myth 3: Celiac disease is easily recognized.
Celiac is very difficult to diagnose. In fact most people are asymptomatic. Symptoms can vary greatly from person to person and can appear at any age.

SUPPORT BLUE CIRCLE DIABETES FOUNDATION
We need your help and support to continue to grow, expand and touch the lives of countless people in the diabetic community. Every little bit helps us in sustaining this endeavour.
Click here to donate

