Summer and Diabetes : Beat the Heat!
As the temperatures soar, it is important to understand how change in weather affects your blood sugars. Have you noticed a lot more hypos or hypers this season? There is no need to let external factors such as the environment have the upper hand always. Here are a few favourite hacks on surviving the hot and brutal summer months while managing your blood sugars :

Hydrate
It is essential to drink enough water to avoid dehydration, especially in the summers. Hot weather, decreased fluid intake, electrolyte imbalances, strenuous exercise and high blood sugars create and add to the perfect storm of dehydration. Dehydration is one of the factors that could result in hyperglycemia and in turn high blood sugars also cause further dehydration, so it is a vicious circle that is best avoided. While water is the best zero carb drink out there, you could also explore various other non caffeinated drinks to stay hydrated. Salted lemonade with soda or water, sparkling water, chaas, jal jeera, flavoured water, infused water (try infusing water with a few slices of lime or cucumbers) are only a few low carb options that might not require a bolus or a minimal one at most. There are many more options and varieties, so do not forget to keep sipping through the heat! Keep in mind that caffeinated beverages might actually dehydrate you and be counter productive.
I have a little rule for myself in my head that might be useful for all the caffeine addicts - for every cup or two of tea or coffee, I must follow it up with a glass of water.

Protect medication
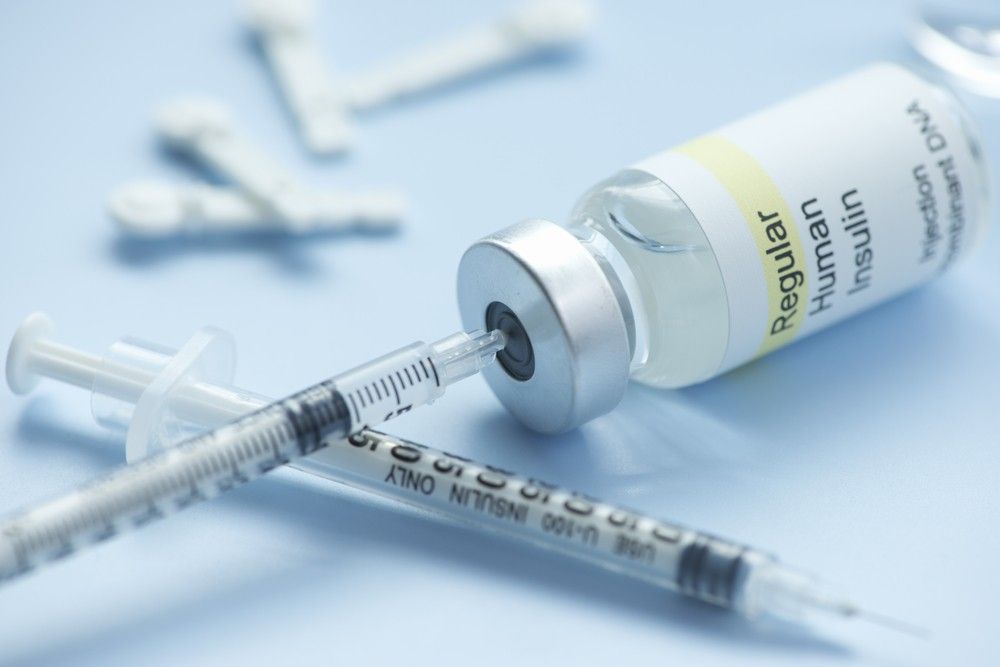
Insulin loses its potency when exposed to heat for too long. This is could lead to 'unexplained' high blood sugars due to ineffective insulin. Insulin not in use must be stored in a refrigerator between 2 to 8 degrees C. While it is fine to keep your in-use insulin at room temperature (between 15 to 25 degrees C) and away from direct sunlight, in temperatures over 25 degrees celsius, it is best to refrigerate insulin, preferably in the butter compartment.

If you are travelling, a Frio pouch is one of the most handy and easy ways to keep your insulin cool. It is available in various sizes and colours depending on your preferences. It is available on most online stores, check it out here.
If you do not have access to a refrigerator or a cooling pouch such as Frio, using an earthen or clay pot also called a 'matka' to store insulin and keep it cool is an affordable and practical solution. Cover the pot with a wet towel or a damp cloth to help it remain cool for longer. Load shedding is common in rural areas and this is a great way to keep your insulin from getting denatured.
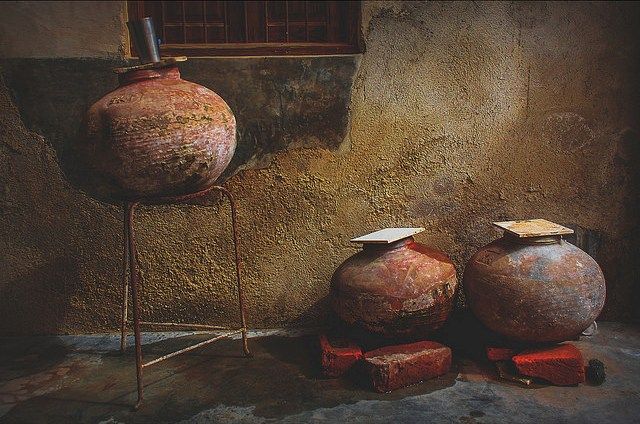
Extreme heat can also affect the effectiveness of other diabetes supplies such as strips, meters and CGMs or FGMs. Avoid leaving them in cars or exposed to direct heat and sunlight. Be vigilant to read and follow the usage guidelines on your products.
Sunburn
Be careful of sunburn as it stresses your body and could potentially increase sugars. Wear loose fitting, light clothes and use sunscreen.
If you use a pump, CGM or FGM, you might find the need for additional taping or adhesives in the summer to avoid it coming off with sweat.

Heat exhaustion
Heat exhaustion can often be confused with hypoglycemia as both have similar symptoms of dizziness, light headedness and irritability among other things, making hypos harder to spot. Also our metabolisms are higher in hot and humid climates, which can lead to higher chances of hypos. Do not disregard hypo symptoms and when in doubt, always test your blood sugar, especially before driving or heading out for a workout.

Exercise
Just because it is hot and uncomfortable, that does not mean you should skip exercise. Exercise is great for absolutely anyone but as diabetics it has got a ton of more benefits for us. Read our guide to exercise and diabetes management here. Pick an exercise time slot that is least hot - either early mornings or evenings. If you need to workout in the afternoons, ensure it is in an air conditioned studio or gym. If your workouts are very intense and causing you to sweat a lot, ensure you replenish salts and electrolytes adequately. Heat combined with exercise could cause hypoglycemia since the heat can cause blood vessels to expand and drastically increase insulin absorption. If you are dehydrated and let's say sprinting or sparring, that could cause you to spike. It is a good idea to take a small break and check BG rather than keep powering through and eventually landing up in a mess because of a hypo or hyper. Always have access to a glucometer, CGM or FGM and keep your hypo stash handy. Needless to say, be smart in your choice of snacks if you usually carry snacks along.
A tip : If you go for a jog right after you take your shot on your thigh, you could most definitely expect a hypo due to the increased blood flow in your legs while jogging.
Test BG often
As the weather changes, it is important to test more often than normal to catch and treat any potential highs and lows. Also, if there is any change in routine it becomes doubly important to check more frequently. Summer vacations might be a time for school kids to wake up late and play longer hours each day, increasing the risk of hypos with the same basal profile used on lesser active school days. Until BG is checked frequently enough to correlate, one would never know where to begin adjustments.

Log
Only testing blood sugars is not going to cut it. You would also need to log it down for it to make sense. Once you do, you will be able to spot patterns and decide what to do about it next. Use the Blue Circle Diabetes mobile app to make logging fun and share the reports with your healthcare provider too.

Dose adjustment
Finally, based on your blood sugar data that you have logged in a format that makes it easy for you to see the different variables at a glance, you can make the much needed dosing decisions and changes as required. For instance, if your meals, doses and activity have been constant over a few days and you are still having more hypos than expected, you could try reducing your basal dose and keep a close eye to see if that solves the issue over the next few days. Read more about basal testing.
Different routine
A change in weather in addition to a change in routine (holidays) makes diabetes management more challenging but not impossible. If you are travelling, remember to carry enough supplies and keep them cool. It might be tempting to give into temptation since you are on a holiday and make detrimental food choices which could lead to uncontrolled blood sugars and putting on unnecessary weight.
I remind myself why I made the choices I did in the first place and I sail through the holiday season smoothly.
Happy holidays everyone!

SUPPORT BLUE CIRCLE DIABETES FOUNDATION
We need your help and support to continue to grow, expand and touch the lives of countless people in the diabetes community. Every little bit helps us in sustaining this endeavour. Our NGO is registered under Section 80G of the Income Tax Act, India.
Click here to donate

